Xeroderma Pigmentosum
Skin Conditions
Xeroderma pigmentosum is a rare genetic disorder in which the body is unable to effectively repair DNA after it has been exposed to ultraviolet radiation found in sunlight, thus resulting in a high rate of genetic mutations and a tendency to develop malignant skin cancers. This disease is autosomal recessive – both parents must contribute one copy of a defective gene for their child to display xeroderma pigmentosum; individuals with only one defective gene are unaffected.
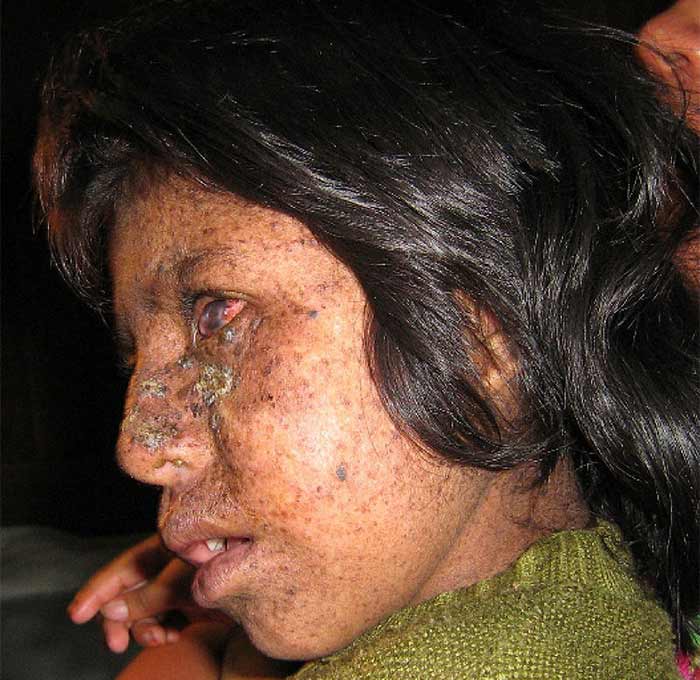
Ultraviolet (UV) radiation is a component of sunlight that results in sunburn. When this radiation meets skin cells it can cause individual subunits of the DNA found in these cells to bind to each other (specifically the pyrimidine thymine). In a healthy persons this damage is efficiently repaired by multiple proteins. However, in the case of xeroderma pigmentosum, defective genes inherited from both the father and mother cause these proteins to become non-functional. Thus, this damage is not repaired and quickly accumulates and results in a greatly elevated rate of UV radiation induced mutations. Unfortunately these mutations often lead to malignant skin cancer including basal cell carcinoma, squamous cell carcinoma, and the deadly melanoma.
Individuals with xeroderma pigmentosum must take great care to avoid exposure to sunlight for even the smallest amount of sunshine will result in extreme sunburn followed by the appearance of multiple actinic keratoses (red flaky pre-cancerous lesions) and other sun-induced blemishes such as freckles. Other signs and symptoms of xeroderma pigmentosum include eyes that are extremely sensitive to sunlight that may become painful and bloodshot following normal sun exposure, the development of poikilodermas (a UV radiation induce skin lesion characterized by pigment changes and telangiectasia/spider veins), and neurological symptoms such as muscle spasms, poor muscle control, deafness, and developmental delay.
Xeroderma pigmentosum is typically diagnosed early in life following extreme sunburn after first exposure to sunlight. Unfortunately, the prognosis for individuals with xeroderma pigmentosum is poor – the extremely high rates of development of malignant skin cancers typically leads to death between ages 20-40. The mainstay of treatment for xeroderma pigmentosum is to avoid sun exposure in the first place followed by aggressive treatment of all skin lesions that develop. Contact your dermatologist if you are worried that you or your child is showing signs of xeroderma pigmentosum.