Treat Alopecia Areata in California
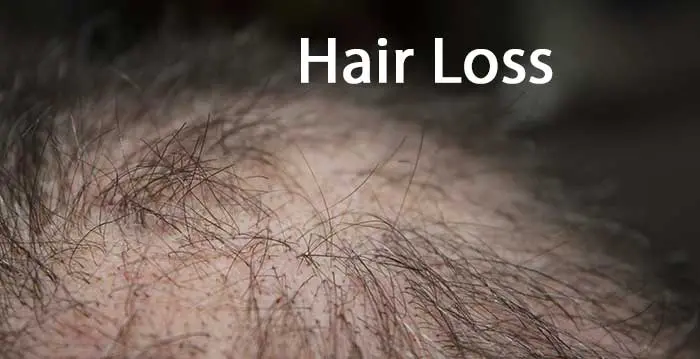
Hair Loss
Contour Dermatology and Cosmetic Surgery Center’s board-certified dermatologists have years of experience addressing hair loss due to alopecia areata. If this condition affects your self-confidence or way of life, we want to offer you the solutions you’ve been looking for.
Treat Alopecia Areata in California
Hair Loss
Contour Dermatology and Cosmetic Surgery Center’s board-certified dermatologists have years of experience addressing hair loss due to alopecia areata. If this condition affects your self-confidence or way of life, we want to offer you the solutions you’ve been looking for.
What Is Alopecia Areata?
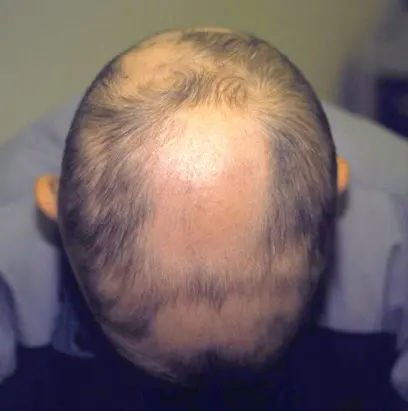
Alopecia areata is an autoimmune disorder that is mostly benign. Though it is often asymptomatic, it is commonly characterized by patchy hair loss on the scalp, eyebrows, eyelashes, beard or anywhere your body grows hair. It starts as a localized patch, but can expand to multiple patches over time. It is usually associated with conditions like:
- Pruritus (itching) and burning sensations in the affected area
- Atopic dermatitis
- Acute or chronic stress
- Vitiligo
- Collagen-vascular diseases
- Thyroid disease
- Down syndrome
- Psychiatric disorders, including anxiety, depression and personality disorders

How Do We Treat Alopecia Areata?
Because the condition is benign and often asymptomatic, treatment is not a requirement to live a healthy life. Still, the team at Contour Dermatology and Cosmetic Surgery Center knows that the potential visible symptoms of alopecia areata can bring emotional or psychosocial upset. We are here to help restore confidence in your appearance and encourage hair regrowth through:
- Intralesional (injectable) corticosteroids: In alopecia areata cases with less than 50% involvement, we recommend injectable corticosteroids in the affected areas. Treatment occurs every four to six weeks, so we can adjust your treatment plan as needed and monitor regrowth.
- Topical corticosteroids: For more involved cases or for patients who are children, we may recommend topical corticosteroids instead. This is a daily ointment that can start regrowth in as little as three months. Patients must stay current with their applications to maintain growth.
These treatments are available for first-time flare-ups and spontaneous recurrences.
Why Choose Contour Dermatology and Cosmetic Surgery Center?
Our staff prides itself on combining medical precision with cosmetic artistry, providing you with wellness services that are as aesthetically pleasing as they are effective. When you come to us, you can rest assured that we will develop a personalized treatment plan that addresses your precise treatment goals and prioritizes results.
As we work on improving the appearance of your alopecia areata, we can also find solutions for some of the associated conditions mentioned above. Your provider can inform you of our full range of services to help your body look and feel better than ever.
Schedule Your Consultation Today
If you’re dealing with unwanted alopecia areata patches, schedule a consultation with Contour Dermatology and Cosmetic Surgery Center today. Our board-certified dermatologists are ready to help you.